Providing timely insights to inform policy tackling women’s health inequalities
Health Medical and public affairs Health economics outcomes research Health equity Life sciences
Case study: Our work with the Royal College of Obstetricians and Gynaecologists (RCOG)
The challenge
The Royal College of Obstetricians and Gynaecologists (RCOG) wanted to build fit-for-purpose recommendations for more equitable solutions to the problems of ever-increasing waiting lists and a historically overlooked health specialty.
The RCOG noted our work on NHS waiting lists during the pandemic, and how women’s health had suffered the most significant indirect impacts of Covid-19, with gynaecology having the highest rate of increase in numbers on the waiting list out of all health specialties.
New policies and a data-driven report were needed to push for action from the NHS to benefit not only female patients, but also those yet to seek care and healthcare staff.
Our approach
From Autumn 2021 to Spring 2022, we worked together with the RCOG to:
- characterise the overall known waiting list by geography and in relation to other specialities;
- estimate the number of ‘hidden referrals’ since the pandemic began – patients who would have been expected to have joined the waiting list in the absence of the pandemic; and
- identify how hospital care for gynaecology has varied since the pandemic by admission type and condition.
We used publicly available NHS data to estimate the number of known patients on the gynaecology waiting list from April 2018 – January 2021 across the UK.
We used historical NHS England data to model expected number of referrals and compared this to the actual number to estimate the hidden referrals (i.e. expected number less actual number).
We provided estimates that were as granular as possible by geography (Clinical Commissioning Group and NHSE region) to enable actionable insights from our analysis.
We also identified the number of gynaecology-related admissions over the last three years broken down by inpatient or outpatient and condition type.
Our findings
At 31 December 2021, over 570,000 patients across the UK were waiting for gynaecological treatment. This is a 60% increase since pre-pandemic levels.
In England, the gynaecology waiting list has increased at the fastest rate (60%) of all specialities, rising to nearly 460,000 as of 31 January 2022.
Geographical disparities between nations and CCGs are clear. This may be linked to Covid-19 rates but other factors may also be involved (the North West was the hardest hit region within England).
Figure 1: Geographical variation of gynaecology waiting list size by region
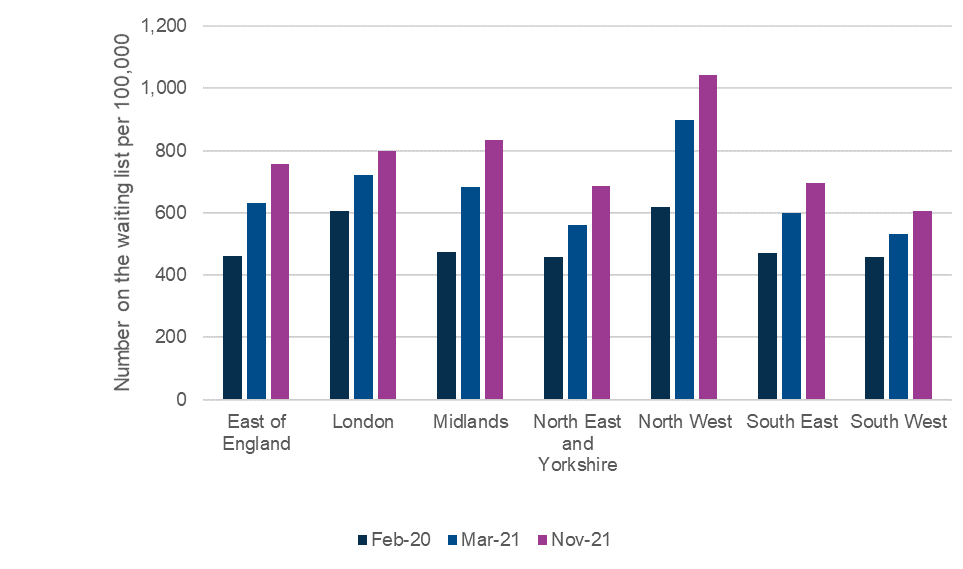
As of 31 January 2022, approximately a further 400,000 patients were estimated to be hidden referrals yet to join the formal NHS waiting list. Consistent with the known waiting list, our estimates suggest this number has large geographical disparities, with the North West of England having the highest burden of hidden referrals.
Urogynaecological conditions appeared to be most impacted by the Covid-19 pandemic, with a reduction of c.60% in admissions for prolapse or incontinence compared to 55% or less for other conditions.
Figure 2: Number of planned admissions by diagnosis type by year
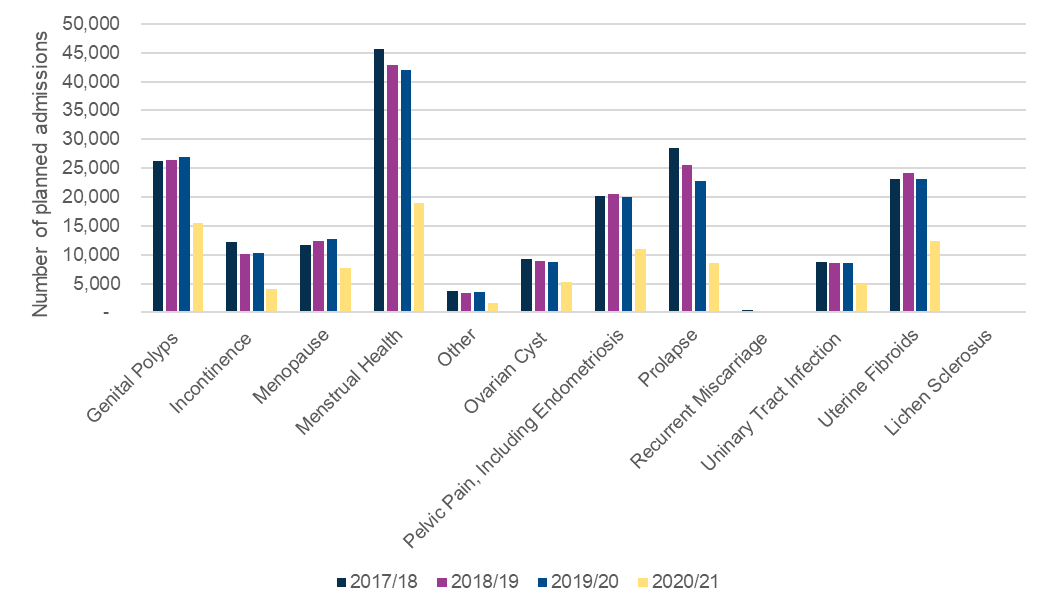
The impact
The RCOG were able to use these findings to support their call for urgent action to address the disparity in referral to treatment times, geographically and by speciality.
Their report, Left for too long – determining the scale and impact of gynaecology waiting lists, called on the NHS to:
- amend how prioritisation of surgery across gynaecology is implemented;
- address the unequal growth of gynaecological waiting lists compared to others in the elective recovery plan;
- focus on reducing geographic disparities in the elective recovery plan; and
- address how staffing may impact and limit the waiting lists across the UK.
This partnership project demonstrated the clear value in using applied analytics to inform our understanding of the disparities in unmet need in light of the Covid-19 pandemic, and to therefore support proportionate and effective resource allocation to mitigate the worsening of health, and wider, inequalities.
Having LCP involved in our report has been of huge benefit. They provided us with great insight that helped us tell the strongest possible story about the unfair impact of the Covid-19 pandemic on women’s healthcare. The team were flexible to changing requirements as the work evolved, and were always on hand to come up with solutions when we faced a challenge.
Rosie Walworth, Policy Manager, Royal College of Obstetricians and Gynaecologists (RCOG)
Find out more about the RCOG Elective Recovery Tracker
Start hereHow can we help you?
Do you have a question, RFP or want to talk? Reach out and we’ll connect you with a member of our team.



