Navigating the NHS: What Life Sciences should consider as a General Election approaches
Health Medical and public affairs Life sciences
A UK General Election is approaching. The Prime Minister must call one by January 2025 or risk parliament automatically being dissolved. ‘The NHS’ is consistently cited as one of the most important issues facing the UK and will be a major battleground topic. Party conferences gave an indication of the issues at the forefront, including waiting list backlogs, workforce shortages, population health and emerging technologies. Many of the promises currently are big on vision but lacking in detail.
The next 12 months will be critical as manifesto pledges are drafted and details agreed. For wider healthcare stakeholders, like the Life Sciences sector, advocating for change in business-critical topics, such as the clinical trial environment, will be a priority. However, Life Sciences should also engage on broader challenges; as partners to the healthcare system, they can underline barriers that are preventing patients from achieving the best possible outcomes, as well as providing solutions. Innovative approaches to evidence generation will be key to highlighting problems and modelling potential scenarios for tackling them.
Reducing the elective-backlog: A cross-party consensus
Never before have elective waiting lists stood as long as now; as of the latest figures, 7.8 million people are waiting for treatment. Delays at this scale are something no government can ignore. Within the broader context of workforce shortages and increasing demand from the more than 50% of adults now living with a complex, chronic disease, improving capacity is a priority. Indeed, the Health Minister and shadow Health Minister both proposed solutions, including new funding pledges, workforce investment, and technologies, such as virtual wards. Life Science companies with technologies that could assist in reducing waiting lists, such as new oral medications for cancer that could be taken in the community rather than in hospital, should emphasise this wider value to policymakers.
Total numbers of those waiting only tell half the story; our own LCP waiting list analysis has revealed, waiting lists are not equitable across the county. As of August 2023, the North West and the East of England remain the areas in the country with the most people waiting for care after adjusting for population size.
Increase in RTT waiting lists, after adjusting for population size, across the UK since March 2020
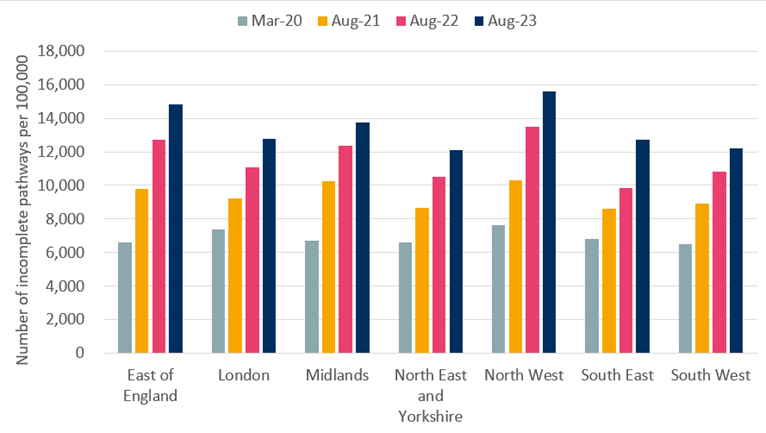
Source: LCP Analysis, Consultant-led Referral to Treatment Waiting Times Data 2023 - 24
By speciality, orthopaedics remains the largest waiting list. Our previous work with the Royal College of Obstetrics and Gynaecology found a 60% increase in gynaecology waitlists since the start of the pandemic in Spring 2022, the biggest percentage change across specialties and a number that has risen since.
These nuanced issues underline the importance of insightful data. Again, this is where partners can play a role, bringing evidence to policymakers to inform and drive change. One area ripe for this is in making the economic case for tackling waiting lists. Our work with the IPPR Think Tank showed that achieving the NHS Elective Recovery plan could deliver economic benefits worth at least £73 billion over five years. With the UK facing stagnating growth and where every public pound should be responsibly spent, articulating how better healthcare can drive economic prosperity would not fall on deaf ears.
An importer of illness to an exporter of health?
History tells us that politicians tend to focus on immediate funding promises for the NHS. At Party Conferences, it was therefore welcomed to see all sides recognise the necessity for wider reform. The NHS was set up on a model of providing care in sickness, in contrast to the health creation model required today shifting care to the community, The Prime Minister recently made one of the biggest announcements for population health in decades with the smoking age to be raised so that ultimately nobody will be able to legally buy cigarettes.
Integrated Care Systems (ICSs) are crucial to improving population health. Much of focus over the next 12 months will likely be on their future development. Indeed, we already see significant variation in the maturity of ICSs across the country. The political debate will undoubtedly focus on finding the right balance between NHS England oversight versus local flexibility. ICSs should provide an appropriate standard of care whilst also prioritising the health outcomes most relevant to the populations they serve.
One core purpose of ICSs is to tackle health inequalities. Life sciences can use data to continue to shine a light on inequalities within their disease areas, for example through post market surveillance after a new medicine is launched. Using data to make the case should mean the complex issue of tackling health inequalities is not lost as a topic in upcoming political debates that can often focus on issues with shorter-term solutions.
Moving from analogue to digital
Technology as an enabler to NHS reform is another area of cross-party consensus. The current Government is championing AI, recently announcing a new £100 million fund to accelerate its use to speed-up drug development in disease areas with high unmet need.
The largest opportunity for AI currently lies in automating the back end of healthcare including logistics, appointment booking and management. The widespread use of AI in health is still controversial with some knotty problems related to regulation, data quality, safety, and patient acceptability. For Life Science companies bringing new technology to the NHS, it is important to be sensitive to these challenges, as we explored in our recent webinar on the topic and articulate their innovation as a way augmenting doctors work, rather than a replacement to human care altogether.
With an upcoming election, the Life Sciences sector is at a critical juncture to be part of the conversation on topics that matter most to health outcomes. The industry can play a role in providing solutions to some of these most imminent health system challenges. The backbone to this will be insightful data, showing where there is the greatest unmet need and helping build consensus for change.
Subscribe to our thinking
Get relevant insights, leading perspectives and event invitations delivered right to your inbox.
Get started to select your preferences.





